Is the baby crying? I opened my eyes. Why is it so bright? I closed my eyes. Shuffling noises. Pain. No, that is not a noise that either of our children make. Where am I? I opened my eyes again. White hospital blanket. I blinked. IV in my arm. Nurses.
I AM ALIVE!!!!
I have never been so happy to wake up in my entire life. It was the most immense feeling of gratitude. I wondered how many days had previously passed where I had opened my eyes without gratitude? From now on, I knew, I would feel grateful for every single day that I was blessed enough to simply open my eyes.
“I need to see my husband,” I told the nurses over and over. “His name is Josh; please go find him.” I couldn’t wait to see his face and show him I was still alive!
After what seemed like an eternity, someone finally escorted that handsome man to my bedside. One of my nurses actually had to keep me in the bed; I couldn’t get into his arms fast enough. That embrace was everything. It said I’m still here, I love you, I’m alive, and everything really is going to be okay. The only words that came out of my mouth, though, were “God is not done with me yet.”

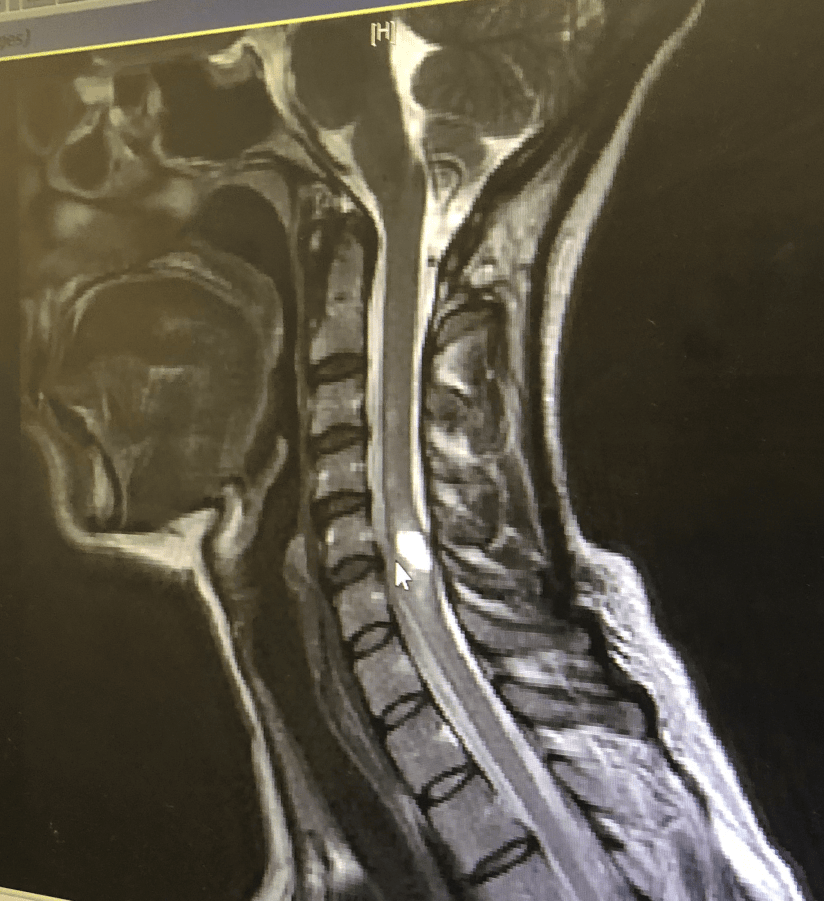
There were so many small victories worth celebrating. Surgery had been successful; it had only taken 4 hours, rather than the anticipated 6. 100% of one meningioma was removed, and 85% of another. Initial CAT scan and MRI showed minor inflammation and no signs of brain bleeding.
I did not have my blood supply severed. I did not have a stroke or seizure in the Operating Room, I did not have any known deficits. It was the best case scenario.
For the first night, I was kept in the Intensive Care Unit (ICU) as my husband (aka Gatekeeper) kept a close eye. We have a huge family and a wide circle of friends, so naturally the room was flooded by visitors. My dad and stepmom even flew in from Kentucky to be with us on surgery day, and help with our boys.
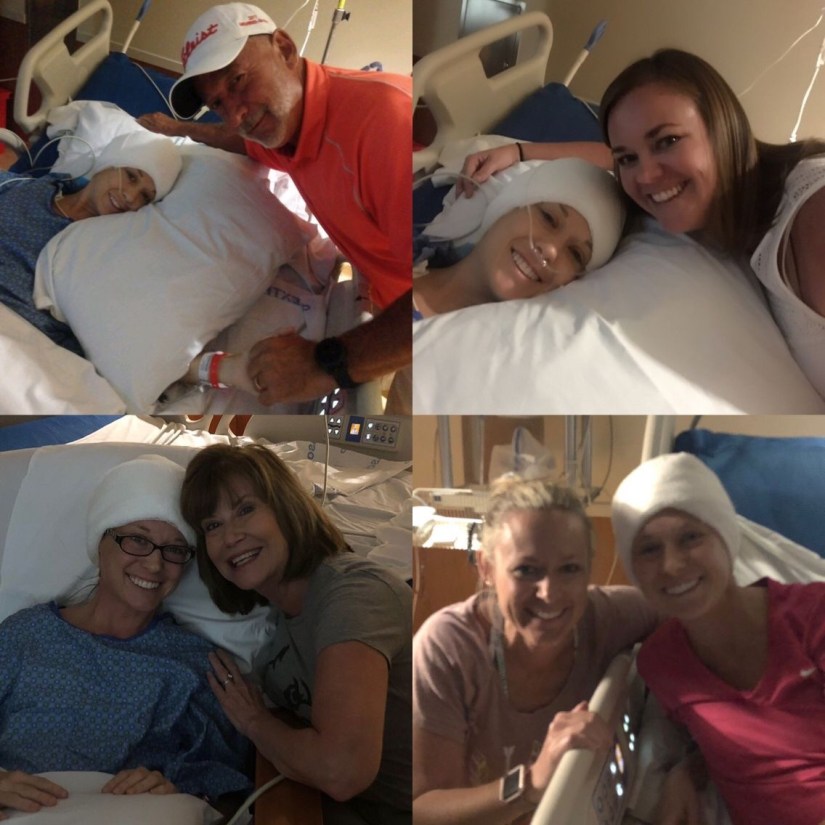
When I remember those first few days after waking up, I don’t remember pain, numbness in my left side, or fear of what might come next. I only remember the LOVE; holding my dads hand like I was a child again; a dozen beautiful white roses; sleeping with Buddy, the bear my boys had made to keep me company; my cousin sneaking a beer into the room for Josh; a friend putting a blue hospital glove on his hand to make me smile; sweet handmade cards from our kids and friends; and my father-in-law revealing he had shaved my name in the side of his head – yes, seriously!! M-E-G (photo below, for proof).

Each act of kindness amounted to something so much bigger; the incredible support system we have standing behind us.
On Day 2, I was released from the ICU to intermediate care. I was able to hold my head up a bit more, and even took a short walk down the hallway, with some assistance. After a nap, Josh and I agreed that our babies could visit. But, I didn’t want them to see me as a sick mom in a hospital bed. So, Josh helped me change out of my hospital gown and into my normal mom-gear (yoga pants and a T-shirt), my nurses agreed to let me ditch the pulse oximeter (for just an hour), and a cousin brought in those sweet rays of sunshine!

After about 10 seconds… it was clear that my act was not fooling either of them. Our oldest hated the IV in my arm, and our youngest kept giving my “hat” funny looks. Eventually, they both let me hug and snuggle them, as long as the IV didn’t come too close.

On Day 3, a team of neurosurgeons woke me up and were ready to remove my “hat.” Since surgery, I had been wondering how much hair was left on my head. Josh had even shaved his head to show support. When the time came, it was like ripping off a band-aid; quick, and so painful I saw stars. My hands instinctually went up. I still had hair, but it felt foreign; it was twisted, tangled, and matted with blood.
The doctor said the incision looked “great,” but I can assure you there is nothing pretty about wearing a headband of stitches (I’ll save you from the gory images here).
It took a dedicated nurse, 2 bottles of awful sterile hospital shampoo, and 4 towels to get my hair semi-clean. Upon starting, the most patient nurse in the world asked if my hair was red. I told her “no, it’s blonde.” Her eyes widened, and she got to work trying to find my hair amid the mess on my head. I watched the water run red for over an hour. My hair was coming out in handfuls. At one point, a few metal staples even fell onto the tile, and washed down the drain. That poor nurse scrubbed for as long as I could tolerate it. When I could no longer hold my head up, I changed into dry clothes, and slept off the pain.
I must have slept for hours; but it’s easy to lose track of time in the hospital. I woke up when that very same nurse came in to announce we were being discharged!
Home!

This is my story, and I’m so grateful that it is not over yet.